What is Medicare Part D?
Medicare Part D is prescription drug coverage available to anyone with Medicare Part A and/or Part B. We cover everything you need to know, including coverage, costs, and eligibility.
The Four Parts of Medicare
Medicare consists of four basic parts: Part A, Part B, Part C, and Part D. Generally, the different parts of Medicare help cover specific services. Depending on your situation, you can get Medicare coverage through a combination of these parts. Our advisors can help determine the combination of these four parts that is right for you.
What does Medicare Part D cover?
Medicare drug coverage (Part D) helps pay for prescription drugs (Rx) you need. Part D plans are offered by private insurance companies and provide prescription drug coverage to individuals living in a plan’s service area.
All plans must cover a wide range of prescription drugs that people with Medicare take, including most drugs in certain “protected classes,” like drugs to treat cancer or HIV/AIDS. A plan’s list of covered drugs is called a “formulary,” and each plan has its own formulary. Medicare drug coverage typically places drugs into different levels, called “tiers,” on their formularies. Drugs in each tier have a different cost. For example, a drug in a lower tier will generally cost you less than a drug in a higher tier.
It's important to know that you must have creditable drug coverage - coverage that is comparable to or better than what is available through Medicare - once you’re eligible for Medicare. Otherwise, you could incur a Late Enrollment Penalty.
There are two ways to get Medicare drug coverage (Part D):
1. Stand-alone Medicare drug plans. These plans add Medicare drug coverage (Part D) to Original Medicare. You must have Part A and/or Part B to purchase a separate Medicare drug plan. Medicare Supplement plans do not include prescription coverage and therefore require enrollees to purchase a separate Part D plan.
2. Medicare Advantage Prescription Drug (MAPD) plans. These Medicare Advantage plans (Part C) roll Part A (hospital-related), Part B (medical-related), and Part D (prescription drug) benefits into one plan.
What does Medicare Part D cost in 2026?
Actual costs of Part D plans, as well as the amount you pay for your medications, are set by the insurance companies, and approved by the government. Your costs will vary based on the medications that you take and the plan you choose.
Most Part D plans include:
- A monthly premium
- An annual deductible
- A prescription drug formulary
- Copays and/or coinsurance per drug
- Coverage phases (Annual Deductible, Initial Coverage Phase, and the Catastrophic Coverage Phase)
What is the Part D donut hole?
The formal term for this period is the “coverage gap.” It refers to a gap in Medicare Part D prescription coverage―a short-term limit on what costs the drug plan will cover. However, with the Inflation Reduction Act, starting in 2026, the donut hole will be eliminated.
Inflation Reduction Act - Changes to Part D: 2026 and Beyond
The Inflation Reduction Act is a significant piece of legislation that includes multiple initiatives. For Medicare beneficiaries, it means significant cost-cutting measures that will affect Medicare Part D for many years to come.
In 2026, a $2,100 out-of-pocket maximum will be implemented for Part D plans. Individuals will have the option to pay out-of-pocket Part D costs in monthly amounts over the course of the year if they choose.
A complete timeline with the Part D provisions of the Inflation Reduction Act can be found here.
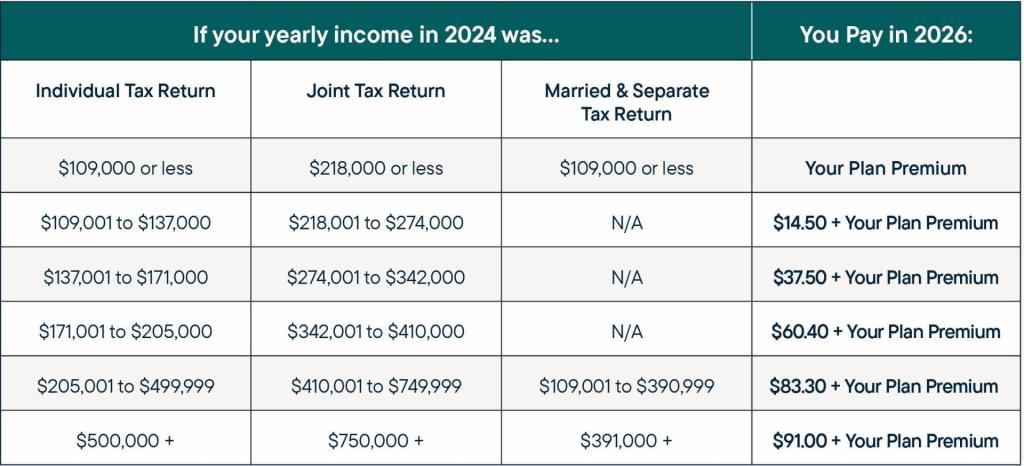
2026 Part D Income-Related Premium Adjustment Amounts
If your income is above a certain level, you will also pay a Part D surcharge. This additional charge is due on top of your plan’s monthly premium.
What is the Medicare Part D late enrollment penalty?
You may have to pay a late enrollment penalty if at any time after your Initial Enrollment Period is over, there’s a period of 63 or more days in a row when you don't have Medicare drug coverage or other creditable prescription drug coverage. The late enrollment penalty is an amount that can be added to your Medicare drug coverage (Part D) premium. You may have to pay the penalty for as long as you have Medicare drug coverage. The cost of the late enrollment penalty depends on how long you went without Part D or creditable prescription drug coverage. Medicare calculates the penalty by multiplying 1% of the “national base beneficiary premium” ($36.78 in 2025) times the number of full, uncovered months you didn't have Part D or creditable coverage. This monthly premium is added to your monthly Part D premium. For more information about the late enrollment penalty and how to avoid it, call our advisors at 888.810.RMED.
Medicare Part D Eligibility
You are eligible for Part D if you’re eligible for Medicare. You must have Medicare Part A and/or Part B to enroll in Part D.
Individuals must be a U.S. citizen or permanent legal resident for at least five consecutive years. You must also meet at least one of the following criteria for Medicare eligibility:
- Age 65 or older
- Are permanently disabled and have received disability benefits for at least two years
- Have been diagnosed with End-Stage Renal Disease (ESRD) or Amyotrophic Lateral Sclerosis (ALS or Lou Gehrig’s disease)
When to Apply for Medicare
Initial Enrollment Period
When you're first eligible for Medicare, you have a 7-month Initial Enrollment Period. If you are eligible for Medicare when you turn 65, you can sign up during the 7-month period that begins three months before the month you turn 65, includes the month you turn 65, and ends three months after you turn 65. We recommend contacting one of our experienced advisors for Medicare advice approximately six months before you turn 65. Learn more about working past 65 and Medicare.
Special Enrollment Period
After your Initial Enrollment Period is over, you may have the opportunity to sign up for Medicare during a Special Enrollment Period (SEP) without having to pay a late enrollment penalty. These are granted due to special circumstances, such as losing or leaving employer coverage.
How to Sign Up for Medicare
If you are not automatically enrolled in Medicare, give us a call at 888.810.7633 and we'll help you understand the steps you need to take and your individual timeline. If you are coming off group coverage, you will want to be sure your Medicare effective date lines up with the end of your other insurance coverage.
When can you enroll in, switch, or drop a Medicare Part D plan?
- Initial Enrollment Period
- Special Enrollment Period
- Annual Enrollment Period (Oct. 15 – Dec. 7)
- Medicare Advantage Open Enrollment Period (Jan. 1 – March 31) when you can change your Medicare Advantage plan to a different one, or switch to Original Medicare (and join a separate Medicare drug plan) once during this time. It is not an option to switch from one stand-alone drug plan to another stand-alone drug plan.

Navigating Medicare Part D: Age-Specific Guidance
The process of choosing Medicare coverage can feel overwhelming, but with preparation and the right partner in Medicare, you will have everything you need to be successful. Here's a simple guide you can reference based on your age and situation.
- Confirm when you’re eligible for Medicare and if you qualify for early Medicare enrollment due to a disability or condition. Take our quiz to find out more.
- Get general Medicare education and answers to your questions by watching or attending one of our live or on-demand webinars.
- Learn about how and when to apply for Medicare.
- Need health coverage now? We offer individual health insurance plans to bridge the gap until you’re eligible for Medicare.
- Learn more about Medicare basics and download your turning 65 Medicare Checklist.
- Call or schedule an appointment with a RetireMed advisor to discuss your unique needs, plans for retirement or for working past 65, and other factors that will determine your specific next steps as they relate to Medicare and the enrollment process.
- Prepare for your appointment with RetireMed.
- Retirement isn’t a requirement to enroll in Medicare. If you’re working past 65, you have many factors to consider as you decide on your health coverage.
- Know specific steps to take and when with our checklist.
- Call or schedule an appointment with a RetireMed advisor to compare your existing coverage to Medicare.
- Navigating Medicare for a loved one can be overwhelming. Remember – we’re here to help answer questions and provide guidance!
- Find out when your loved one is eligible for Medicare and if they qualify for early Medicare coverage due to a disability or certain condition. They can take our quiz to learn more.
- Call or schedule an appointment for you and your loved one to meet with a RetireMed advisor to discuss your loved one’s unique situation.

Working Past Age 65 and Medicare Enrollment
Retirement is not a requirement for enjoying the benefits of Medicare. Many individuals aged 65 and older are delaying retirement and staying in the workforce. If you’re working past age 65, you can sign up for Medicare regardless of your current employment status.
We make it easy to enroll in Medicare without retiring. Our advisors provide personalized guidance to help you choose the health plan that is right for you.

Questions? Your local partner in Medicare has answers.
If you have questions about your plan options or deferring Medicare Part A, contact our team of advisors in Dayton and Cincinnati.